This disease is not well understood, although thousands of observations on subsequent diagnosis and treatment have been described.
The variety and nonspecification of the clinical picture of small pelvic varicose veins leads to large errors in the diagnosis, which will later affect consequences.
Features of small pelvic varicose veins
The veins of the pelvis are many times longer than the arteries, resulting in greater capacity. This is due to the vegetative proliferation of the vascular system of the pelvic region. The pelvic veins are highly adaptable and able to be repaired, contributing to a tangled network.
The speed and direction of blood flow is controlled by valves that are controlled by complex humoral mechanisms. Pressure balancing valves in different parts of the venous network.
When the valves no longer function, the blood becomes stagnant, leading to vascular pathology and varicose veins. The uniqueness of the pelvic veins lies in the fact that, the wide ligaments of the uterus, keeping the lumen wide can narrow it, causing pathology.
Cause of what happened
Pathological pelvic varicose veins can be due to the following reasons:
- Disruption of blood sugar;
- Lubrication of venous stems;
- Compression of accessory bodies by changing the position of the uterus, for example, in reflux;
- ovarian venous valve deficiency (congenital or acquired);
- Post-renal obstruction syndrome;
- Connective tissue pathology;
- Cellular dysplasia;
- Sitting for a long time, working hard;
- Varicose veins of the lower extremities;
- Pregnancy (3 and up) and childbirth (2 and up);
- Diseases of the female genital area (chronic ovarian inflammation, ovarian tumors, fibroids and genital endometriosis);
- Adhesion of the pelvic organs;
- Obesity.
Classification by disease severity
According to the size of the varicose veins, the following degrees are distinguished:
- up to 0. 5 cm, lock the vessel "cork";
- 0, 6-1 cm;
- more than 1 cm.
Variants of the course of the disease
- varicose veins of the perineum and vaginal vestibule; syndrome
- venous obstruction of the small pelvis;
Symptoms
- Most common - frequent pain in the lower abdomen, perineum after prolonged static and dynamic stress. The pain increases in the second phase of the cycle, after hypothermia, fatigue, stress, exacerbations of various diseases.
- Feeling "out of place, " pain during and after sex.
- Menstrual pain - irregular periods, including pain.
- Secretion, more than usual, of gonads.
- Stasis of blood gases leading to infertility, miscarriage, and stillbirth.
- Violation of incontinence due to dilatation of the bladder veins.
Diagnosis
The diagnosis of only complaints is successful in only 10% of cases.
Touching the inner walls of the pelvis, tapering buttons and venous nodes can be palpated. When looking in the mirror, the vaginal mucosa is purple.
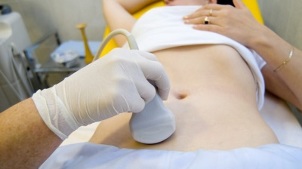
The selected procedure is an ultrasonic examination with color Doppler mapping, which allows the detection of not only ovarian varicose veins, but also venous thrombosis, post-thrombosis. Ultrasound revealed turtle-shaped, "worm-like" structures, with no signal reflection, localized on the lateral surface of the uterus.
The Doppler effect is based on blue and red "shades", the respective venous and artery blood flow.
An ultrasound tester with the help of a special program detects the movement of blood from the sensor and in the other direction, calculates the blood flow velocity and pulse type.
But the exact definition of a vein or artery remains with the doctor. The Doppler method works in almost all cases, the exception to the rules is dictated by our bodies, since the blood flowing from the heart is not always an artery and vice versa.
Thus, an ultrasound doctor will see this artery or vein, the size, the rate of blood in it and many indicators that the average person does not need, but plays an important role. in diagnosis. For this, transvaginal and transvaginal sensors are used.
In 5, 7% of cases, the disease is found by chance during screening. The normal diameter of vena ovarica is 4. 0 cm.
CT and MRI are highly accurate. With these methods, one can detect an accumulation of varicose veins in the ligaments of the uterus, ovaries and around these organs. Pathology can be identified simultaneously.
A very reliable method is phlebographic research.
Contrast is done at the height of the Valsalva assay, as opposed to the blood stream. This allows you to accurately see the valve failure.
Left reconstructive endoscopy, renal lung scan, super-selective phleboovarios endoscopy, and bilateral phleboovariography were also used. These methods help identify hemodynamic and anatomic changes in the kidney veins and the places where the gonadal veins fill them.
Ultra-selective endoscopy is performed by placing a catheter of the gonadal veins through the thigh or subclave, followed by an injection of contrast.
Most of the blood from the uvine tangle veins is poured through the ovary veins. But in hypertensive conditions, it occurs through the ectopic veins into the inner pelvic vein. Varicose veins, where drainage can occur, include sacral and bladder plexus.
In left phleboovaricography, there are 3 stages of venous stagnation in the uviform tangles of the left ovary:
- There is no outflow from the tangle of the left ovary or it follows an additional short path.
- There's an additional long path.
- Two additional output paths or an additional and auxiliary line can be seen.
In stages 2 and 3, varicose veins of the uviform plexus of the ovaries must be formed.
Laparoscopy is used for differential diagnosis. Pathological winding veins are located in the ovarian region, in the direction of the circular and broad ligaments. They look like large blue aggregates with a thin and stretched wall.
The complexity of the diagnosis lies in the fact that the disease is often hidden behind signs of inflammatory processes, various clinical manifestations, camouflage of endometriosis, prolapse of internal organs, pathology. Neurology after surgery and many ectopic diseases.
Treatment
The main goal of treatment is to eliminate intravenous reflux. In the early stages of the disease, conservative treatment is used. In the later stages of the disease, surgery is the treatment of choice.
Treat with caution
It includes normalization of venous tonicity, improvement of hemodynamics and nutritional processes.
Symptomatic treatment for individual symptoms. Nonsteroidal anti-inflammatory for pain relief, bleeding treatment - hemostasis.
The main drugs in conservation treatment are antidotes and anti-platelet aggregation drugs.
Phlebotonics - improves the tonicity of the vessel wall and increases blood flow. With this disease, it is better to consult with your gynecologist about some medicines.
Physiotherapy is an important method.
Surgical treatment
- Cut varicose veins.
- Gonado-caval shunting.
- Sclerosis of the laparoscopy.
- Clear the ovary vein with intravascular x-ray.
Folk remedies
Since the main factor leading to the onset of the disease is the weakness of the valve apparatus, folk remedies for lower limb varicose veins are also applied to this pathology.
The most commonly usedare: hazelnuts, hops, nettle, horse chestnut, dandelion root, kombucha, willow, oak, St. wort. John, vines, pollen and many other plants.
The following are effective: a bath with oak, chestnut, willow, chamomile, medicinal, cayenne, St. John's wort, wire.
Precautions
- The first thing to do if you have a complaint, prediction, or the diseases listed above is to contact your gynecologist.
- Need to normalize working and resting mode, try not to keep straight posture for a long time, being too physical.
- Do preventive exercises "pedal", "birch stand", "scissor leg"
- Follow the diet: eat foods rich in vitamins E, P, C, try to eat only white meat, low-fat meats, replace with fruits, vegetables, whole grains.
- Drink plenty of water, but no less than 1. 5 liters per day.
- Eliminate excess weight, bad habits.
- Consult your doctor about wearing compression clothing, it will improve the flow of blood from the lower extremities, thereby reducing congestion in the small pelvis.
- Avoid bathing, saunas, steam rooms, hot showers.
In order not to have such a difficult disease to diagnose, you need to follow the precautions listed above. Consider your health the most precious thing in life.
For the smallest suspicious symptoms that you cannot heal within a few days, you should see your doctor. He must give you highly qualified help and save you from suffering.





































