Varicose veins, also known as varicose veins, in daily life are often referred to as "fatigue of the legs". But in reality, the factors that cause it are much more complicated. And the disease itself is not at all just a harmless cosmetic defect. Varicose veins of the lower extremities lead to the appearance of chronic venous insufficiency - a condition, the end result of which can be the appearance of a venous feeding ulcer.
Of course, in the majority of cases we are dealing with moderate varicose veins, which are now effectively and practically treated, without recurrence. But first things first.
Why is varicose veins dangerous?
How common varicose veins is, difficult to say: many patients consider this a cosmetic defect and do not seek medical attention. According to the statistics of Western scientists, at least a quarter of the population in the United States and Europe has this disease. In our country, the disease has been recorded in over 30 million people. At the same time, according to some studies, no more than 18% know about their condition, and no more than 8% receive treatment.
Varicose veins of the lower extremities is a disease in which the structure of the vein wall is altered. The vessels lengthen, contract, in areas of thinning, the lumen dilates, forming nodes.
Statistics
Varicose veins are hereditary diseases. Its probability of occurrence in family members with no venous disease is no more than 20%. If either parent has the disease, the risk increases: for men - up to 25%, for women - up to 62%. When both parents have the disease, the child has a 90% chance of developing varicose veins.
With varicose veins, the ratio of the two main structural proteins of the vein wall is disturbed:collagenandelastin. . . If collagen forms stiffness, then elastin, as the name implies, is responsible for elasticity - the ability of the vein wall to return to its original state. In patients with varicose veins, the amount of this protein in the vein wall is reduced. The collagen itself also changes: instead of the common type III collagen, which is responsible for elasticity, the content of collagen type I - stiff, retains residual deformation, increases. In addition, the number of smooth muscle cells that regulate the lumen also changes, the ability to interact between them is impaired. These pathological changes are hereditary in nature. Then the game started playingexternal factors:
- static loads for a long time - the need to stand or sit motionless;
- overweight;
- pregnancy and childbirth.
Some experts point to chronic constipation, tight clothing that increases intra-abdominal pressure, and high heels that interfere with the normal functioning of the muscle pumps in the legs as predisposing factors.
Individually or in combination, these factors increase pressure in the venous system of the lower extremities. The altered vein wall no longer "holds" pressure, the vein lumen dilates. Due to the dilation of the venous lumen, the valves, which supply blood flow in only one direction, stop working. IncurredReflux- reverse flow. The pressure inside the affected vein even increases, and the vicious cycle is closed.
Increased venous pressure, combined with changes in the wall's structure over time, triggersinflammatory response- initially only on the valve surface and the inner wall of the vessel. Gradually, inflammatory proteins and blood cells begin to "see" through the damaged vein wall into the surrounding tissue. There they are destroyed, releasing active substances -Inflammatory mediators. . . They damage surrounding cells and attractwhite blood cellshas the function of removing damaged tissue. The result is edematous, calloused and hyperpigmented skin of the feet. These processes can cause venous nutrition ulcers. Prolonged inflammation of the vein wall also increases blood clotting. In combination with venous congestion, this leads to the fact that blood clots begin to form in the dilated vein. Incurredthrombophlebitis- another dangerous complication of varicose veins.
Manifestations of varicose veins are divided into objective and subjective.Subjective symptoms- here are the patient complaints about:
- heaviness in the legs;
- rapid fatigue;
- paresthesia - unpleasant sensations of "goose bumps", changes in sensitivity;
- feeling of heat in the muscles;
- leg pain, the characteristic feature of which is a decrease in intensity after walking;
- swelling in the evening;
- restless legs syndrome - leg discomfort that prevents you from sleeping;
- night cramps in the lower extremities.
The combination of these symptoms and their severity is individual and does not always correlate with changes in the vein wall and surrounding tissues.
The combination of subjective complaints and objective changes in the tissues of the lower extremities forms the basis of the modern classification of varicose veins and chronic venous insufficiency:
- C0- there are complaints, but there is no change in appearance, lesions of the veins can be detected only on special examination and examination;
- C1- Appearance of "spiders" (scientific name - telangiectasias) or a network of varicose veins in the skin (reticular varices) becomes evident;
- C2- the diameter of the dilated hemispheric veins exceeds 3 mm, the appearance of dilated nodes;
- C3- the affected leg becomes persistently swollen;
- C4- changes appear in the surrounding tissues: darkening of the skin (hyperpigmentation), development of eczema, induration of the subcutaneous tissue;
- C5- the period when the ulcer has healed;
- C 6- stage of open ulcer.
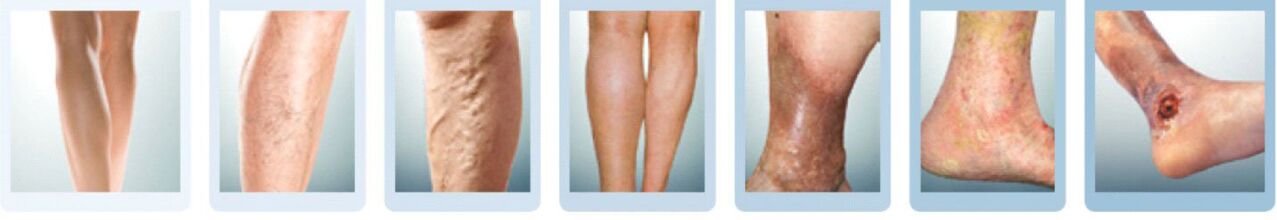
Starting from the fourth stage, the nutritional skin changes described can no longer be completely eliminated. Even cured varicose veins at this stage will not lead to complete resorption of the hyperpigmentation or induration. In addition, it should be remembered about a rather dangerous complication -thromboembolism. . .
On a note
Between 30 and 60% of deaths due to deep vein thrombosis of sudden onset and further thromboembolism against the background of venous insufficiency associated with thrombophlebitis go undetected and untreated.
Therefore, you should not delay the treatment of varicose veins until later, especially against the background of the achievements of modern veinology.
Modern methods of treating varicose veins
Methods and techniques that meet several criteria can be considered modern: minimally invasive (traumatic), highly effective, low likelihood of recurrence and complications, and short rehabilitation period.
- Conservative therapy.This includes the use of compression knitwear, ointments and venotonics (oral medications). Current clinical guidelines suggest that oral venotonics can reducesubjectivemanifests (complaints) in the early stages of the disease and reduces edema, but in no way affects the state of the vein wall itself. Different ointments have the same effect. Arnica compress is considered a very effective treatment for varicose veins, as it reduces the manifestations of venous insufficiency, alleviates the patient's subjective complaints and prevents the progression of insufficiency. vein. However, compression knitwear is unlikely to cure varicose veins - varicose veins will not function properly.
- Traditional surgical resection.The affected large or small hemispheric vein is tied where it drains into the deep venous system, where it is then removed with a special metal probe. This operation is effective, but is quite painful and takes a long time to recover. There is a high probability of postoperative complications - hematoma, postoperative paresthesia and neuralgia.
- Therapy therapy.A special drug is injected inside the varicose vein, which helps to "glue" its walls. This procedure is less traumatic and is recommended for the treatment of small diameter veins. However, it is rarely used to remove the dormant stem of large and small saphenous veins, as it is characterized by a higher rate of recurrence. In addition, such an unpleasant complication as hyperpigmentation in the framework of scleroderma may occur.
- Endovenous laser coagulation (EVLK)- The method of treatment of varicose veins by minimally invasive method, safe, modern and effective. It has synonymous names: endothelial laser ablation, intravascular coagulation of the veins of the lower extremities, endothelial laser opacification (EVLO). But whatever the name, the laser coagulation technique is the same. A radial fiberoptic light guide is inserted through the perforation into the vein. Then, with the help of a special pump, an anesthetic solution is pumped around the vein, which not only anesthetizes the procedure, but also compresses the vein, reducing its diameter and thus protecting it. surrounding tissues from overheating. For this procedure, a modern vascular laser is used, which produces two waves: one of them is absorbed by the hemoglobin in the blood, the second - by the vessel wall. Vienna is "brewing beer". All phases (position of the led light, permeation of the solution around the vein, the "phase" process itself) are monitored in real time using the ultrasound device. The duration of the EVLK procedure on one limb is 30-60 minutes.
It's important to know!
The only effective treatment for varicose veins is to remove the altered portion of the vein that is no longer able to perform its functions.
Advantages of laser removal:
- Minimal trauma, allowing the procedure to be performed on an outpatient basis and under local anesthesia;
- you can go home right after surgery;
- quick recovery;
- good cosmetic results: leaving no marks and scars;
- High efficiency, low recurrence rate.
As endothelial laser coagulation is currently considered one of the most advanced, minimally invasive and minimally invasive treatments for varicose veins, we will consider this technique in more detail.
Indications for laser coagulation
The primary indication is varicose veins, independent of the diameter of the vein stem and its anatomical options. The scope of indications of EVLK can be extended due to the perfection of modern equipment - two-wave laser, radial fiber.
Contraindications to the procedure
In most cases, they translate to a severe somatic condition of the patient:
- deep vein thrombosis (obstruction, occlusion, obstruction);
- decompensated type 1 diabetes mellitus;
- severe atherosclerosis and ischemia of the lower extremities;
- severe cardiovascular diseases: ischemic heart disease, in particular, angina at rest, large-scale myocardial infarction with decreased cardiac output, severe forms of arrhythmia, stroke;
- severe coagulopathy, both descending and ascending;
- pregnancy and lactation;
- individual intolerance to the anesthetic used;
- inability to do physical activity immediately after the procedure;
- inability to use compression knitwear.
It is such a feature that the age of the patient is not a contraindication.
How is laser coagulation of a vein done?
A short time before manipulation, it is recommended to purchase compression stockings at the 2nd degree of compression (25–32 mm Hg). Your doctor will tell you the required size details. Endovasal laser coagulation itself does not require any special preparation.
All stages of endovenous laser blinding are performed under the control of continuous ultrasonic waves.
- Before starting the procedure, the vein is "marked": the doctor makes a mark on the skin, corresponding to the places where the blood flows backwards, the branches that flow into the veins.
- At the beginning of the operation, under local anesthesia, the vein is punctured (perforated). The sensations are no different from that of a regular intravenous injection. A radial light guide is inserted into the vein using a special catheter.
- Next, a protective "sleeve" of the anesthetic is created around the vein. Under ultrasound control, using a special pump, the doctor injects a local anesthetic into the space around the vessel. This not only allows pain relief, but also protects surrounding tissues from the excess heat of the laser.
- The procedure itself is EVLO varicose veins. In modern optical fibers, laser radiation is delivered uniformly around the entire circumference of the device, which helps to heat the vein evenly from the inside. After removing the light guide plate, the patient underwent ultrasound to monitor the condition of the treatment vessel, as well as the deep veins of the extremities.
- A compression garment is placed on the patient.
Immediately after the end of the manipulation, the patient should go for a walk, lasting at least 40 minutes.
Possible complications
Some of them are few, only temporary, and the likelihood of complications is mainly related to the use of outdated medical equipment and low qualifications of doctors.
- Deep vein thrombosis -may occur in patients with a predisposition to thrombosis. Therefore, to prevent this complication, patients are prescribed drugs that reduce blood clotting. As a rule, they are used within 4-5 days after the intervention.
- Thrombophlebitis- usually associated with inadequate laser irradiation.
- Pigmentation along the treated veinwithin 1, 5–2 months.
- Feeling of "tight" veins- pass within 1, 5 months.
To prevent the development of any complications as much as possible, you should adhere to a few simple rules, the observance of which is necessary for successful rehabilitation.
Rehabilitation
On the first day, there may be aches and pains along the vein. To get rid of them, ordinary pain relievers are enough. The temperature may rise for the first few days. Just using traditional means to reduce it is enough.
In general, for successful rehabilitation, 2 main conditions should be observed - wearing compression underwear and maintaining adequate physical activity.
- Compression underwear -in the first 5 days, it is not eliminated even in one night of sleep. This is necessary for the vein to "glue" and heal completely. Moreover, compression knitwear is worn only during the day. Just wearing compression garments for 2. 5–3 months is sufficient, but if risk factors are present (sedentary, long standing work, use of female sex hormones), additional prophylactic knitwear is recommended. .
- Physical activity- Walk for at least an hour a day. But you will have to give up intense sports for about a month.
During the month, you should avoid hot baths, baths and saunas.
Evaluate the effectiveness of the method
Analysis of foreign and domestic publications shows that the effectiveness of laser varicose vein treatment ranges from 93 to 100%. The failure can be attributed to several groups of factors:
- anatomical features of the vein to be operated on;
- violation of the technique of performing EVLK (insufficient laser power, insufficient venous compression with anesthetic solution);
- the patient's non-compliance with the rules of the postoperative regimen (usually - refuse compression).
The immediate and long-term results of laser coagulation of the lower extremity veins are better than radiofrequency ablation and sclerotherapy, and are comparable to traditional surgical techniques. At the same time, laser treatment of varicose veins has a much better tolerability, shorter rehabilitation time, and less number of complications compared with classical surgical approaches.
How much does EVLK cost?
The endovasal laser coagulation procedure requires high-tech equipment and expensive disposable consumables (lamps), which explains its cost. The total amount will depend on the volume and complexity of the procedure, the medical equipment used, and the doctor's qualifications.
Therefore, endoscopic coagulation laser is a modern effective treatment for varicose veins. It gives excellent clinical results and, in fact, leaves no residue. Minimal trauma from exposure allows you to return to the normal life (with minor limitations) already on the day of surgery, without requiring a hospital regimen and any special conditions for recovery.
How to choose a clinic?
A vascular surgeon, veniologist says:
"The outcome of lower extremity laser coagulation depends largely on the expertise of the medical staff, as well as on the technical characteristics of the equipment used. This means that the equipment is used. The application must be modern, and the doctor must be qualified. So I would recommend choosing a clinic that specializes in this particular type of service, has been in business for several years and has a longstanding reputation. "





































